Therapy of Mamma Carcinomas – Especially BRCA-Tumors
Therapy of mamma carcinomas – there are many and they can be quite complex. Many conditions play a role, such as the exact diagnosis, the age, the genetic predisposition, the general physical and mental condition, and yes, unfortunately sometimes also the financial possibilities. In this article we deal specifically with BRCA mutation-positive tumors, for hormone-associated tumors please see here!
Therapy Options in BRCA-Breast Cancer
BRCA breast cancer is a form of breast cancer caused by a mutation in one of the two BRCA genes. These genes are important for repairing DNA damage that can lead to cancer. Women with a BRCA mutation have an increased risk at age 40-50 of developing breast cancer. Treatment options for BRCA breast cancer depend on several factors, including staging, hormone receptor and HER2 status, age, and the patient’s desire to have children.
Surgery
A surgery is probably the most important therapy of mamma carcinomas. It involves removing the tumor from the breast, sometimes along with the lymph nodes in the armpit. There are different types of surgery, such as breast-conserving surgery (lumpectomy), mastectomy (removal of the entire breast), or bilateral mastectomy (removal of both breasts). Women with a BRCA mutation are at higher risk for recurrence or a new tumor in the same or different breast. Therefore, bilateral mastectomy may be an option to lower the risk. However, this surgery is not suitable for every woman and also has disadvantages, such as loss of natural breast tissue and possible complications. An alternative option is regular monitoring of the breasts by mammography and magnetic resonance imaging (MRI).
Chemotherapy
Chemotherapy is a treatment with drugs designed to inhibit or kill the growth of cancer cells. It is often used after surgery to destroy any remaining cancer cells and reduce the risk of recurrence. This is called adjuvant chemotherapy. Chemotherapy is also sometimes given before surgery to shrink the tumor and make surgery easier. This is called neoadjuvant chemotherapy. Chemotherapy may also be used for advanced or metastatic breast cancer to control tumor growth or relieve symptoms. Chemotherapy is usually given in cycles, with breaks in between to give the body time to recover. The type and duration of chemotherapy depends on the patient’s individual situation. The most common drugs are anthracyclines (e.g., doxorubicin) and taxanes (e.g., paclitaxel). Chemotherapy also has side effects, such as nausea, hair loss, fatigue, or infections.
Hormone Therapy
Hormone therapy is a treatment for women with hormone-dependent breast cancer, i.e. whose tumors have receptors for estrogen or progesterone. These hormones can promote tumor growth. Hormone therapy works either by blocking the action of these hormones or by lowering their levels in the body. Hormone therapy is often given after surgery or chemotherapy to reduce the risk of recurrence. It may also be used in advanced or metastatic breast cancer to control tumor growth or relieve symptoms. Hormone therapy is usually taken for several years. The most common drugs are tamoxifen, aromatase inhibitors (e.g., anastrozole), or GnRH analogs (e.g., goserelin). Hormone therapy also has side effects, such as hot flashes, mood swings, weight gain, or osteoporosis.
PARP-Inhibitors
PARP inhibitors are a new class of targeted drugs approved specifically for women with BRCA mutation and HER2-negative breast cancer. This inhibitor is an enzyme involved in DNA damage repair. PARP inhibitors block the function of PARP, preventing cancer cells from repairing their DNA. This leads to cell death of the cancer cells, while the healthy cells are less affected. PARP inhibitors are used as monotherapy, i.e. without combination with other drugs. They are taken in tablet form. The only approved PARP inhibitor for breast cancer is olaparib (trade name: Lynparza®). It can be used in women with locally advanced or metastatic breast cancer who have previously received anthracycline/taxane-based chemotherapy and possibly hormone therapy.
Olaparib has been shown in a clinical trial to prolong progression-free survival (the time without tumor growth) compared with standard chemotherapy. It also has a higher response rate and better quality of life than chemotherapy. Olaparib also has side effects, such as anemia, nausea, vomiting, diarrhea or fatigue.
Further Therapy of Mamma Carcinomas
In addition to the above therapies, there are other treatment options for women with BRCA breast cancer that may be used depending on the individual situation. These include:
Radiation Therapy:
Radiation therapy is a treatment using high-energy radiation to destroy tumor tissue. It is often used after breast-conserving surgery to reduce the risk of breast recurrence. It may also be used for advanced or metastatic breast cancer to control tumor growth or relieve symptoms.
Immunotherapy:
Immunotherapy is a treatment designed to activate or boost the body’s immune system to fight cancer cells. There are different types of immunotherapies, such as antibodies (e.g., atezolizumab), checkpoint inhibitors (e.g., pembrolizumab), or vaccines. Immunotherapy is usually used in combination with other drugs. It is not yet approved for all breast cancer patients, but is only available for certain subtypes or in clinical trials.
Bisphosphonates:
Bisphosphonates are drugs that inhibit bone resorption and can thus reduce the risk of bone fractures and bone pain. They are often used in women with metastatic breast cancer whose tumor has spread to the bones. They may also be used in women with hormone-dependent breast cancer who are receiving hormone therapy and are at increased risk for osteoporosis.
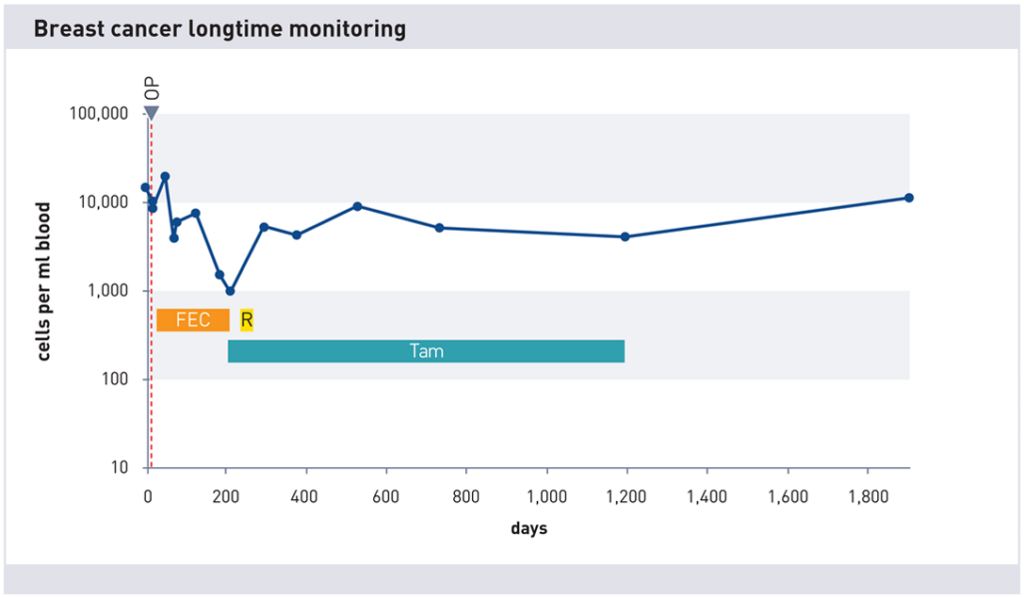
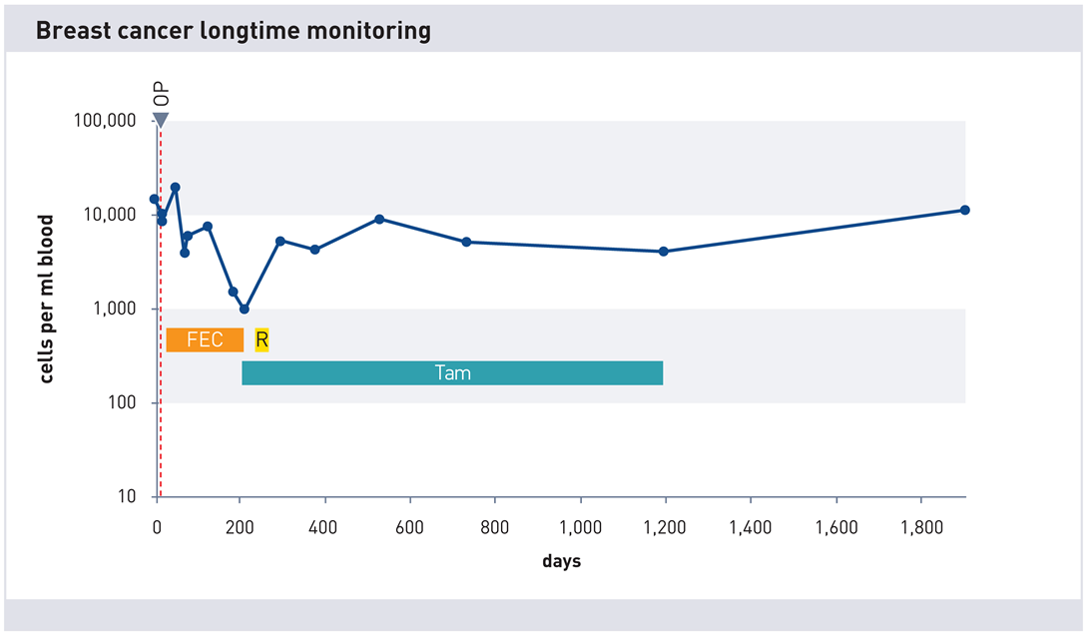
Repeated measurements of cell count at different times during therapy
maintrac Blood Collection Sets for surveillance of a cancer therapy
With maintrac it is possible to detect an increase in tumor cell count at an early stage. This should be done regularly (every ~6 months). This way, measures can be taken in time if necessary. If you decide to use maintrac, you can order a blood collection kit here on our partner site youcann.de!
Conclusion
The therapy options for BRCA breast cancer are diverse and depend on various factors. The decision for a particular therapy should always be made individually, taking into account the advantages and disadvantages, as well as the patient’s personal preferences. Close cooperation between the patient and the treatment team is therefore important to ensure the best possible care.